Continuous Monitoring for Provider Demographics and Credentialing Data
Daily Checks
Across all active providers
Immediate Alerts
For sanctions and changes
Both Streams
Demographics and credentialing
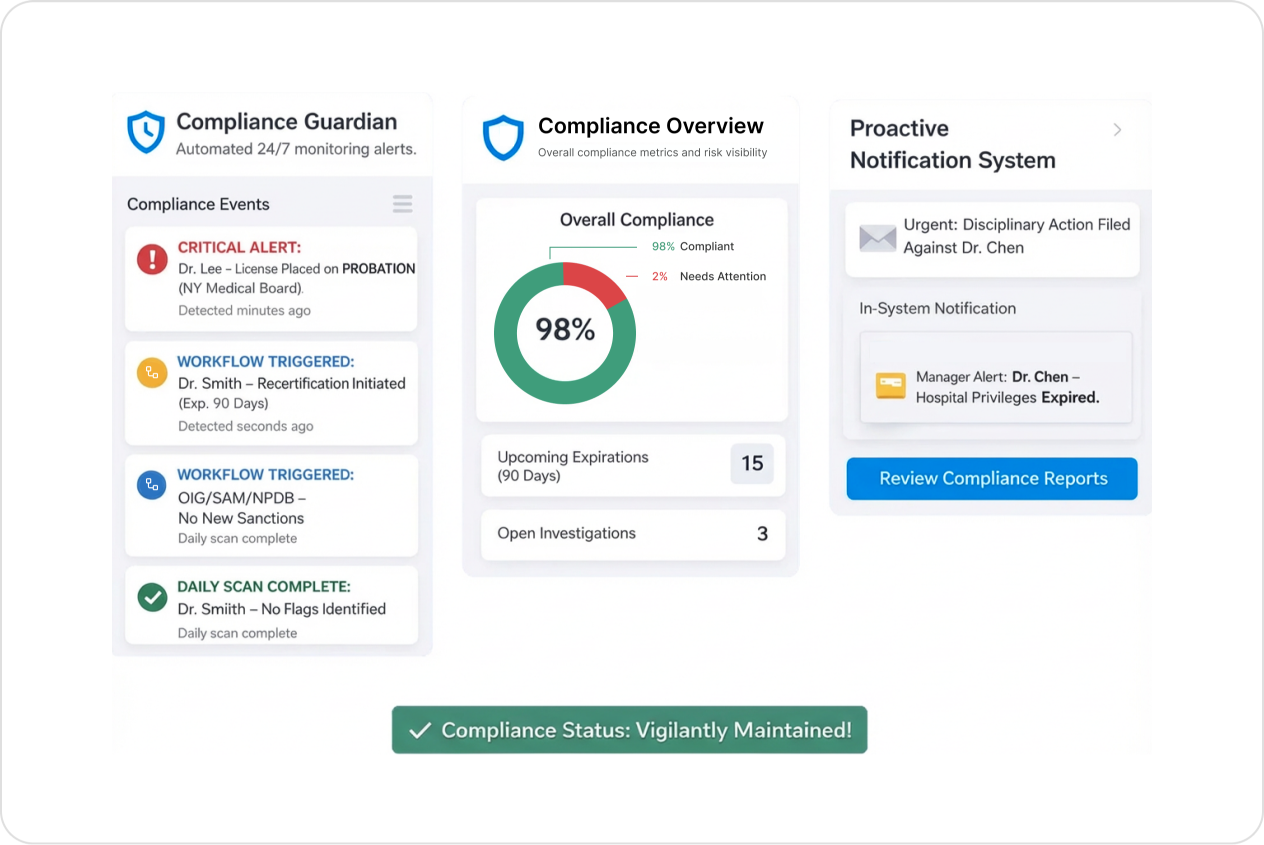
Credentialing Happens Once. Providers Change Every Day After That.
Demographic Changes Go Unnoticed
Providers update locations, contact details, or panel status, but directories remain outdated because nothing triggers a re-check.

Compliance Gaps Between Cycles
License issues or sanctions can occur mid-cycle and remain undetected until the next review or a claim denial.

Manual Monitoring Does Not Scale
Checking exclusion lists and license boards across large provider networks consumes time and never keeps up with ongoing changes.
PRIME® Monitors Demographics and Credentialing Data, Continuously and Automatically
Two monitoring streams. One platform. No gaps between your scheduled verification cycles.
[01] Demographics Monitoring
Track Every Practice-Level Change
- Monitors provider addresses, phone numbers, fax numbers, and contact details continuously
- Detects office relocations, practice closures, and affiliation changes as they happen
- Flags telehealth availability updates, panel status changes, and hours modifications
- Queues confirmed changes for directory update without waiting for the next scheduled cycle

[02] Credentialing Data Monitoring
Catch Compliance Events Between Re-Credentialing Cycles
- Screens against OIG LEIE, SAM.gov, and all 50 state Medicaid exclusion lists continuously
- Detects license probations, suspensions, and revocations from state medical boards in real time
- Monitors DEA registration status, board certification standing, and hospital privilege changes
- Flags new disciplinary actions and adverse events the moment they appear on any source

[03] Automated Alert Workflows
Route Every Alert to the Right Team Instantly
- Tiered severity routing sends critical alerts such as sanctions immediately to compliance leads
- Lower-priority demographic changes queue for scheduled review without creating noise
- Configurable notification rules by provider type, credential category, and organizational role
- Every alert is logged with the source, timestamp, and resolution action for audit documentation

[04] Cross-System Data Consistency
Keep Every Connected System Current
- Validates provider data consistency across credentialing platforms, directories, and claims systems
- Flags discrepancies between your internal records and authoritative sources such as NPPES
- Pushes confirmed updates to connected systems automatically without manual intervention
- Maintains a full change history showing what was detected, when, and how it was resolved

Complete Documentation
- Monitoring logs showing which databases were checked, when, and what was found per provider
- Demographics change history with source confirmation and directory update records
- Credentialing event records documenting every sanction, lapse, or status change detected
- Alert resolution trails capturing team response, action taken, and system update confirmation

Continuous Provider Credentialing Monitoring Software - FAQs
What is the difference between demographics monitoring and credentialing monitoring?
Demographics monitoring tracks practice-level changes such as addresses, phone numbers, panel status, and affiliation updates. Credentialing monitoring tracks compliance events such as license status changes, sanctions, DEA expirations, and disciplinary actions. PRIME® runs both streams continuously so neither type of change falls through the gap between scheduled review cycles.
How often do monitoring checks run?
Sanctions and exclusion list checks run daily across all active providers. License status and credential checks run daily for high-priority providers and on a configurable schedule for others. Demographic monitoring runs continuously against provider websites and authoritative sources. Monitoring frequency is configurable by provider type and organizational policy.
Does continuous monitoring replace re-credentialing?
No. Re-credentialing is a comprehensive verification event that runs on a defined cycle, typically every three years. Continuous monitoring is what protects your organization in the time between those cycles, catching the changes that a periodic review would not discover until it was too late.
How are detected changes pushed to downstream systems?
Once a change is confirmed and resolved, PRIME® pushes the updated record automatically to connected systems including credentialing platforms, provider directories, and claims systems. Every update carries a timestamp and source attribution for full traceability.
What compliance standards does continuous monitoring documentation support?
PRIME® generates monitoring reports for CMS Medicare and Medicaid continuous screening requirements, NCQA ongoing monitoring standards, Joint Commission surveillance requirements, and state-specific jurisdiction mandates. Documentation is exportable for regulatory audits at any time.
What is continuous credentialing monitoring?
Continuous credentialing monitoring is an automated verification process that tracks provider licenses, sanctions, exclusions, DEA registration, and board certifications in real time between recredentialing cycles. Instead of waiting for the next three-year review, it runs daily checks against OIG LEIE, SAM.gov, state medical boards, and all 50 state Medicaid exclusion lists, so compliance events surface the moment they appear.
How does continuous credentialing monitoring work?
The platform runs daily automated queries against authoritative sources including OIG LEIE, SAM.gov, state medical boards, DEA registries, and state Medicaid exclusion lists. When it detects a license suspension, sanction, exclusion, or disciplinary action, it triggers tiered severity routing so critical alerts reach compliance leads immediately. Every check is logged with source attribution and timestamp, building an audit-ready record without any manual effort.
Why is continuous credentialing monitoring important?
Credentialing happens once. Provider status changes every day after that. A license can be suspended, a sanction can be issued, or a DEA registration can lapse mid-cycle, and without continuous monitoring, organizations do not discover these events until the next scheduled review, sometimes years later. That gap creates exposure to CMS penalties, NCQA findings, claim denials, and patient safety risk tied to unauthorized providers.
What should continuous credentialing monitoring cover?
Strong monitoring covers OIG LEIE and SAM.gov exclusion lists, all 50 state Medicaid exclusion databases, state medical board license status including probations and revocations, DEA registration, board certification standing, hospital privilege changes, and new disciplinary actions across any authoritative source. Leading platforms also extend into demographic monitoring, catching address changes, panel status updates, and practice closures that affect directory accuracy.
How is continuous monitoring different from recredentialing?
Recredentialing is a comprehensive verification event that runs on a defined cycle, typically every three years, to reverify every data point in the provider file. Continuous credentialing monitoring is what protects your organization in the time between those cycles, catching license suspensions, sanctions, and exclusions the moment they happen rather than waiting for the next scheduled review to discover them.
How does PRIME® continuous credentialing monitoring support compliance?
PRIME® runs daily screening across OIG LEIE, SAM.gov, and all 50 state Medicaid exclusion lists, plus continuous checks against state medical boards, DEA, and board certification sources. Alerts are routed by severity, with critical events like sanctions reaching compliance leads immediately while lower-priority changes queue for scheduled review. Every check carries a timestamp and source, generating CMS, NCQA, and Joint Commission-ready documentation that stays audit-ready at any moment.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)

