No Surprises Act Regulations: What Health Plans Are Still Getting Wrong in 2026

Data Quality in Healthcare: Why It Matters for Providers & Payers


10 min read | Last Updated: 13 Mar, 2026
TL;DR
- Alarming misidentification rates: 10% of incoming hospital patients are misidentified, risking wrong treatment from data entry errors; 8-12% duplicate records create confusion, resource waste, and care delays across healthcare systems.
- Six quality measurement criteria: UK government identifies accuracy (correctness), completeness (all necessary information), consistency (uniform formatting), validity (rule compliance), uniqueness (no duplicates), and timeliness (up-to-date status) as data quality measures.
- Poor data threatens clinical trials: Inaccurate patient information directly affects clinical trial reliability; missing or wrong data can falsely show treatments as beneficial or harmful, influencing approval decisions with far-reaching patient health consequences worldwide.
- PRIME® achieves 95% validation: Atlas PRIME uses primary source validation with direct health system outreach, convenient self-service provider portals, and AI-driven Ask PRIME tool delivering 95% data validation success rates for trusted payer information.
Summarize This Article With
Every decision in healthcare, whether it’s diagnosing a condition, prescribing medication, or coordinating treatment, relies on one critical factor: data quality. The consequences can be serious if that data is inaccurate, incomplete, or inconsistent.
And there's a number to prove it. 10% of incoming patients are misidentified at hospitals. That means one in ten patients could be at risk of receiving the wrong treatment simply due to a data entry error.
And it doesn’t stop there. Most hospitals deal with duplicate records ranging from 8% to 12%, creating confusion, wasted resources, and care delays. The more fragmented the data sources, the higher the chances of duplicate records.
So, how do we fix it? By improving data quality. And the best way to do that? Automation. Stick around to see how data quality management can be the life-saver healthcare desperately needs.
What Is Data Quality Management In Healthcare?
Data quality in healthcare refers to the accuracy, completeness, consistency, and reliability of patient and provider data used in clinical, operational, and regulatory processes. High-quality healthcare data supports better patient care, regulatory compliance, and informed decision-making across healthcare organizations.
Good data quality directly impacts:
- Patient safety and care: Ensuring doctors have the right information to make the best decisions
- Interoperability: Making sure different healthcare systems can share and understand data seamlessly
- Regulatory compliance: Meeting legal and industry standards to protect patient information
- Operational efficiency: Reducing errors and delays in hospital workflows
- Research and innovation: Supporting medical advancements with high-quality data
- Decision-making and strategic planning: Helping healthcare leaders make informed choices for better patient outcomes
The Importance of data quality in healthcare
Poor data quality can have serious consequences in healthcare. When patient records contain errors, missing details, or inconsistencies, they can lead to misdiagnosis, incorrect treatments, and compromised patient care.
Beyond individual patients, unreliable data can also skew research findings, making studies less accurate and harder to reproduce.
High-quality data is also important for public health monitoring. If the information collected isn’t accurate, it becomes harder to track disease patterns, plan resources, or respond effectively to health crises.
How to measure quality in healthcare data?
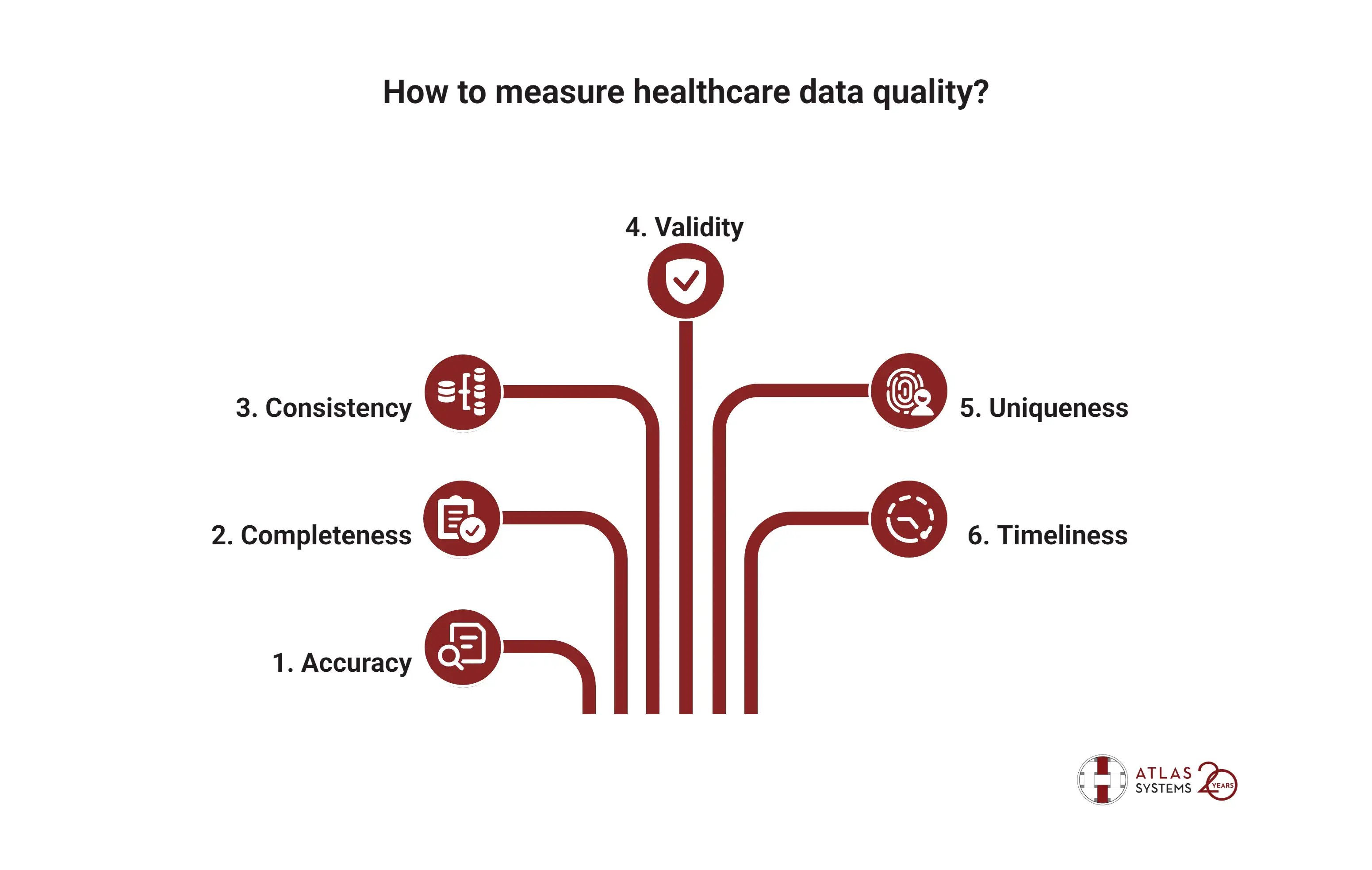
To measure data quality, the UK government identifies six key characteristics:
- Accuracy – Is the data correct?
- Completeness – Has all necessary information been recorded?
- Consistency – Is the data collected and formatted similarly across systems?
- Validity – Does the data comply with business rules and regulations?
- Uniqueness – Are there duplicate or conflicting records?
- Timeliness – Is the data up to date and relevant?
Key Components Of Data Quality In Healthcare
The key components of data quality management are healthcare data governance, standardization, validation, monitoring, and staff training. At an organizational level, effective data governance operates within a broader healthcare governance framework. Governance establishes how leadership teams, boards, and executives define accountability, approve data policies, and oversee risk across clinical, operational, and digital systems—ensuring data quality initiatives are aligned with compliance requirements, patient safety goals, and long-term organizational strategy Together, these form the backbone for ensuring that the data used in patient care is accurate, secure, and consistent.
Data governance
Data governance sets policies, procedures, and clear responsibilities, ensuring data stays trustworthy, protected, and respectful of patient privacy.
In healthcare, it promotes accountability by defining how information should be managed across the entire organization.
Standardizing data collection processes
Standardization means using the same data elements and coding systems across multiple platforms or departments. When information is gathered in a consistent format, it’s easier to combine and analyze.
This approach reduces the chance of errors or misunderstandings, ultimately supporting better clinical and administrative decisions.
Data quality monitoring and reporting
Monitoring involves keeping track of metrics like accuracy and completeness. Reporting goes hand in hand with this process, offering straightforward dashboards highlighting emerging issues.
If errors spike, teams can spot them quickly and address them before they grow into a larger problem.
Data validation and verification
Data validation and verification are methods that confirm the reliability of healthcare data. Examples include cross-referencing with trusted sources or using statistical analysis to catch anomalies.
When you check for inconsistencies or outliers, healthcare organizations can correct mistakes and maintain high-quality data.
Training staff
Everyone on the team must understand the importance of precise information. Training sessions help professionals recognize best practices, keep up with the latest standards, and foster a culture that respects data integrity.
Benefits Of Good Data Quality In Healthcare
Good data quality reduces operational costs, wasted time, and confusion. For example, if a hospital uses accurate patient records from the start, there’s less chance of ordering duplicate tests or dealing with billing errors.
Your organization could be next in line to lose millions each year due to incomplete or incorrect information.
Boost market competitiveness
Competition is growing among hospitals, government agencies, and private companies. High-quality data plays a significant role in attracting patients and improving reputation.
For instance, a clinic that consistently tracks and analyzes patient feedback can refine services, meet patient needs more effectively, and ultimately stand out in the market.
AI capabilities
Artificial intelligence has enormous potential in patient care and administrative processes. For instance, an AI-driven system might analyze symptoms to suggest treatment options for chronic conditions.
However, AI tools depend on large volumes of trustworthy data. If the records contain errors, the technology may produce misleading recommendations.
Centralizing data storage
Some organizations still store medical information in separate databases, making it difficult for doctors, nurses, and administrative teams to share insights. Consolidating these records into a single system removes barriers to collaboration.
A unified platform means fewer overlooked details, for example, a physician can quickly access a patient’s imaging results, lab tests, and medication history without switching between multiple applications.
Improving decision-making through data alignment
Aligning different data sources allows teams to form a clear, holistic view of patient care. When payers and providers share consistent information, it becomes easier to coordinate treatments and manage costs.
Examples Of Poor Data Quality In Healthcare
Here are some examples of data quality issues in healthcare you need to be aware of:
Security of data
Protecting sensitive information, particularly in healthcare, poses significant challenges. Numerous laws govern data storage and management, and violations can be costly.
For example, if a computer containing patient records is stolen from an insurance company, the fine may reach millions.
Switching to cloud-based solutions is often a safer alternative since the vendor typically handles most security-related tasks.
Degraded patient care
Healthcare providers need a complete view of patient information to deliver effective treatment. However, multiple providers, labs, and pharmacies often scatter the data, creating gaps in knowledge and complicating timely, coordinated care.
For instance, if the systems do not integrate, a patient’s primary care physician might miss critical details from specialist visits. This oversight may lead to unnecessary appointments, delays in diagnosis, and inefficient care pathways.
Impact on clinical trials and research
Inaccurate data can directly affect the reliability of clinical trial outcomes. Researchers rely on correct patient information to determine whether a new treatment is safe and effective.
Missing or inaccurate data might falsely show a drug to be beneficial or harmful, influencing important decisions about its approval. This can have far-reaching consequences for patient health worldwide.
Difficult to achieve interoperability
Effective healthcare relies on a seamless flow of information between providers, payers, and patients.
Electronic health records improve data sharing, but organizations still struggle to achieve full interoperability when they store information in different formats or use unstandardized terms. When you harmonize these formats, you can create a unified patient record they can trust, simplifying treatment coordination and reducing errors.
Resource wastage and inefficiency
Insufficient access to patient records often forces healthcare providers to repeat tests and procedures, driving up costs and placing extra burdens on patients.
For example, if a physician cannot find recent lab results, they might order the same tests again, adding expenses for both the healthcare system and the patient.
Over time, this pattern contributes to significant financial strain and unnecessary use of resources, ultimately diminishing the quality of care.
How to overcome these data quality challenges?
Healthcare data accounts for a significant portion of the world’s information, and its volume continues to grow. When this data is spread across multiple systems and organizations, it is often inconsistent, incomplete, or out of date. High-quality data is vital for ensuring that every decision made in healthcare is based on accurate, trustworthy information.
Read More: Overcoming Provider Data Management Challenges
The only solution that you can invest in to combat this is provider data management platform.
So why does a strong provider data management solution matter?
Maintaining updated and accurate provider information is a major undertaking. Payers often struggle to keep up as providers change roles or locations, and providers themselves are typically busy and receive requests from multiple payers.
This problem can result in out-of-date contact details and limited engagement from provider offices.
Falling behind in regulatory compliance or failing to manage provider data effectively can result in fines, reputational damage, and a poor plan member experience.
A strong provider data management solution helps payers maintain and verify provider details, such as specialties and availability so that their patients receive timely, effective care.
How PRIME® Solution By Atlas Addresses These Challenges
Atlas’ PRIME® solution relies on primary source validation which is a proven method grounded in direct outreach to health systems, provider groups, and independent practitioners.
Atlas has refined this process over many years, achieving better results at a lower cost than many health plans would on their own. PRIME® also helps payers satisfy federal (CMS) rules, state regulations like CA SB137, and the No Surprises Act. In addition, it supports emerging interoperability standards such as FHIR.
What is impressive is that the providers remain at the center of this process. Here’s how PRIME helps with managing quality healthcare data:
- Offers convenient, user-friendly channels for provider attestation, including a modern self-service portal. These resources typically result in a 95% success rate for data validation, meaning payers can trust the information they receive.
- The Self-Service Portal (SSP) enables providers to review and correct their own data. Instead of wading through hundreds of columns, they see only the most relevant details.
- PRIME® also features a browser-based dashboard that presents near real-time findings and attestation updates in a single view. An AI-driven tool, Ask PRIME, allows users to query the data with conversational prompts and receive insights in seconds.
So why choose our PRIME solution over other solutions or, better yet, manually doing it?
- Verified, high-quality data: Our system validates provider data at its source, minimizing errors
- Reduced provider abrasion: It works according to providers' preferences, reduces frustration, and boosts engagement
- Compliance made easier: PRIME keeps pace with complex regulations at both the federal and state credentialing levels.
If you have any questions or would like to learn more about how Atlas can support your specific data management needs, feel free to get in touch. We are here to simplify the challenges of provider data management and set you on the path to better outcomes.
FAQs About Data Quality In Healthcare
1. Which type of data is most commonly used in healthcare?
The most commonly used type of data in healthcare is structured data, which is primarily stored in Electronic Health Records. This includes patient details like medical history, diagnoses, prescriptions, and treatment plans, all organized in a standardized format to ensure accuracy and easy retrieval.
2. How is data quality measured?
Data quality is measured by evaluating how well the data serves its intended purpose. This is done using key metrics such as accuracy, completeness, consistency, timeliness (how up-to-date the data is), validity (alignment with required formats and standards), uniqueness (eliminating duplicates), and fitness for purpose.
3. What is the KPI for data quality?
A data quality KPI is a measurable indicator used to evaluate how well data meets reliability and usability standards. These KPIs help generate a data quality score, providing insight into data sources' overall health.
4. Why data quality matters in healthcare
Accurate healthcare data is essential for patient safety, regulatory compliance, and operational efficiency. Poor data quality can lead to misdiagnosis, billing errors, duplicate records, and delays in care delivery, making data governance and validation critical for healthcare organizations.
.png?width=869&height=597&name=image%20(5).png)
-1.png?width=486&height=315&name=IDC%20Banner%20(1)-1.png)
.png?width=300&height=175&name=Rectangle%2034624433%20(2).png)



















.webp)












.png)

