Centralize Provider Data Management Across Every System, Every Team, Every Workflow.
95%+ Accuracy
Automated data quality
Real-Time
Error detection and correction
Continuous
Provider Data Monitoring
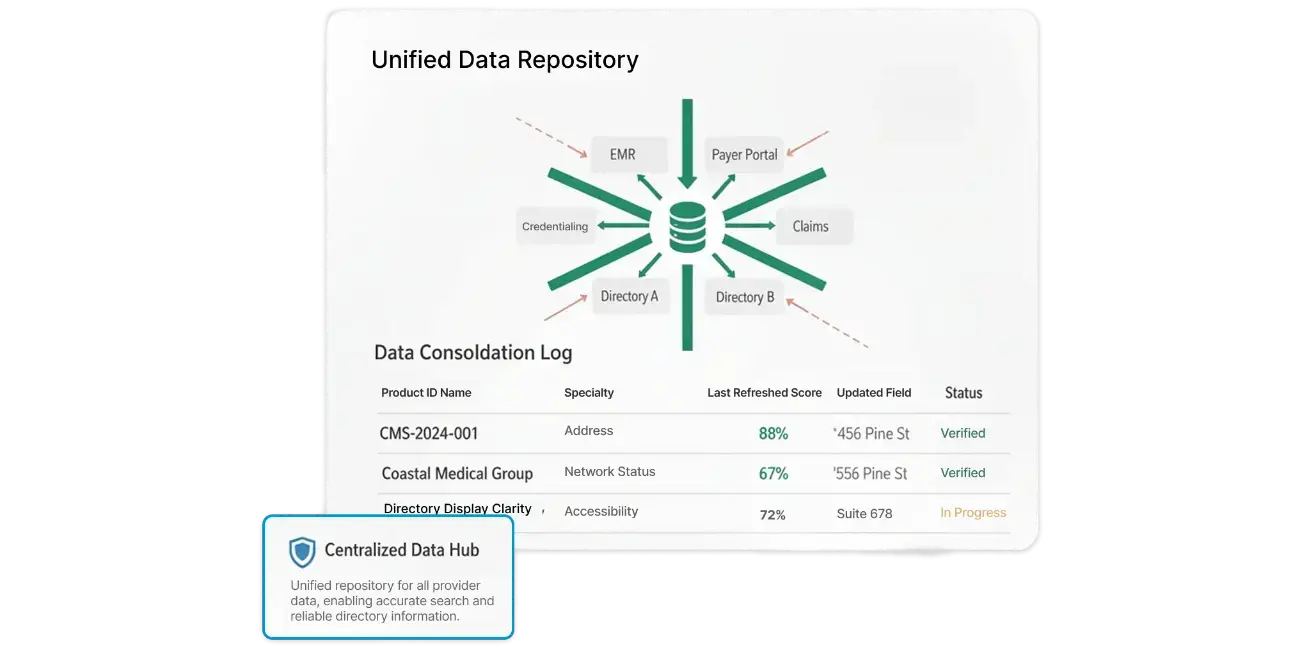
The Provider Record Is
the Most Referenced Data
in Your Organization.
Multiple Systems, Multiple Answers
Your credentialing platform, claims system, and directory each hold a different version of the same record. Every team reconciles independently, and errors still reach patients and payers.

Updates That Never Fully Propagate
A change logged in one system rarely reaches the others. By the time reconciliation runs, the data has changed again.

No Audit Trail Without Manual Work
When regulators request a data change history, most organizations reconstruct it manually from multiple sources.
One governed platform where provider information is always current, always consistent, and always audit-ready.
[01] Comprehensive Profiles
Complete Provider Records
- NPI, DEA, licenses, certifications, specialties, and education
- Locations, phone, fax, email, hours, telehealth status, and panel availability
- Network participation, contract terms, delegated group affiliations, and reimbursement tiers
- License status, sanctions, credentialing standing, and last validation date

[02] Search and Filtering
Find Any Provider Instantly
- Query across any combination of demographic, network, or credentialing fields
- Save frequently used searches for recurring operational needs
- Export lists, reports, and data files without manual compilation
- Bulk correction capabilities let you resolve similar errors across multiple providers simultaneously

[03] Role-Based Dashboards
The Right View for Every Team
- Network Operations: coverage gaps, adequacy status, and contract renewals
- Credentialing: expiration dates, primary source verification queues, and committee status
- Compliance: validation scores, exception flags, and audit readiness indicators
- Trend analysis identifies which data elements degrade fastest and require more frequent attention

[04] Automated Integration
One Record, Every System
- Connects with credentialing platforms, claims systems, EHRs, and CRMs
- Pushes validated data to online and print directories from the same governed source
- Integrates with CAQH, NPPES, state licensing boards, DEA registries, specialty boards, and sanctions databases
- FHIR, HL7, and X12 EDI support with configurable sync rules and full audit trails

Complete Documentation
- Regulatory compliance documentation for CMS, state regulators, and accreditation bodies
- Quality metrics tracking accuracy rates, error types, and correction turnaround times
- Audit trails showing what changed, when, why, and who approved each correction
- Validation evidence confirming primary source verification for every data element

FAQs
How does PRIME® integrate with existing systems?
PRIME® uses industry-standard protocols including FHIR, HL7, and X12 EDI, with pre-built connectors for platforms such as Salesforce, Workday, CredentialStream, and CAQH. Custom integrations for claims, EHR, and directory systems are configured during deployment.
Can different teams have different levels of access?
Yes. PRIME® supports granular, role-based permissions that control data visibility and editing rights by team function. Network operations, credentialing, compliance, and provider relations teams each work within their defined scope.
What happens when data from two sources conflicts?
PRIME® applies confidence scoring to flag conflicts and surface them for review. Your team determines which source takes precedence for each data type, and the system documents that resolution with a complete audit trail.
What happens when the system cannot determine the correct value?
Uncertain corrections queue for manual review with full context on why the record was flagged and what options are available. PRIME® escalates ambiguous situations rather than applying an unverified update automatically.
How often does validation run?
High-priority changes such as sanctions, license status, and demographic updates trigger real-time monitoring. Comprehensive validation cycles run on a scheduled basis, with updates propagated automatically to all connected systems.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)


.png?width=1490&height=152&name=Group%202087329257%20(1).png)