Ad-Hoc Provider Directory Audits That Find Compliance Gaps Before Regulators Do
Zero Findings
Pass CMS audits
70% Faster Fixes
Guided remediation
Complete Proof
Regulatory documentation
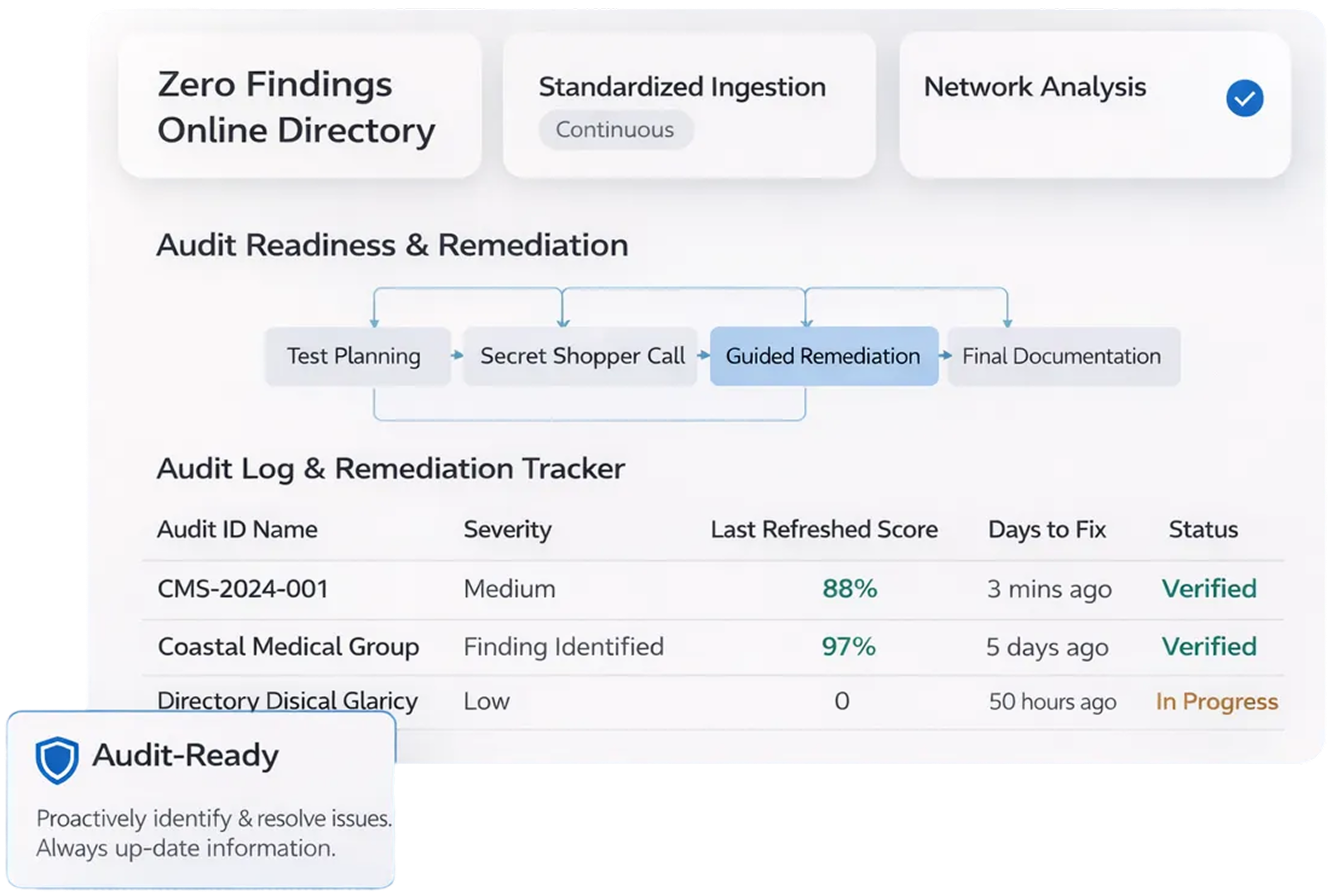
Reactive Data Validation Leaves You Exposed to CMS Findings
Gaps Surface Only During CMS Reviews
Directory issues often appear during secret shopper audits, when remediation windows are already closed and findings are locked in.

Sampling Misses Systemic Issues
Small sample checks fail to detect patterns across regions, specialties, or delegated groups that regulators consistently uncover.
Findings Trigger Real Consequences
CMS audits lead to CAPs, penalties, and Star Rating impact; NCQA findings affect accreditation, all avoidable with early detection.
PRIME® Simulates CMS, NCQA, and State Audit Methodology, On Demand
Identify compliance gaps with enough time to remediate, document, and demonstrate readiness before any formal review.
[01] Mock CMS Testing
Replicate Exactly What Regulators Test
- Random sampling methodology matches CMS secret shopper approach and statistical requirements
- Phone accuracy testing verifies provider connectivity and office responsiveness
- Acceptance status confirmed directly with office staff during outreach
- Wait time, location accuracy, and network participation status verified per CMS standards

[02] Network Gap Analysis
See the Patterns a Random Sample Cannot Reveal
- Comprehensive testing across provider types, specialties, geographic regions, and delegated groups
- Risk scoring prioritizes providers requiring immediate attention before the next audit window
- Trend analysis identifies whether network accuracy is improving or deteriorating over time
- Geographic analysis surfaces systematic issues concentrated in specific markets or service areas

[03] Guided Remediation
Fix Findings on Your Schedule, Not a Regulator's
- Automated re-validation workflows trigger immediately for every flagged provider record
- Exception queues route complex cases with specific resolution instructions to the right team
- Real-time progress tracking shows remediation status across every open finding simultaneously
- Escalation protocols ensure high-priority issues receive immediate leadership visibility

[04] Regulatory Documentation
Walk Into Every Audit With Evidence Already Assembled
- Timestamped logs document every test conducted, finding identified, and action taken
- Evidence packages include call recordings, verification sources, and methodology records
- Remediation records show original finding, correction made, and re-validation confirmation
- Compliance reports demonstrate continuous proactive monitoring for CMS, NCQA, and state reviewers

FAQs
How does a mock audit differ from the CMS secret shopper survey?
The CMS Appointment Wait Time Survey is conducted annually on a fixed schedule with results submitted to CMS by May 31. A mock audit uses the same methodology but runs on your schedule, with results visible only to your team, giving you time to remediate findings before any formal regulatory review occurs.
How many providers are tested in a typical mock audit?
A standard quarterly mock audit tests 100 to 200 providers using random sampling that matches CMS statistical methodology, plus targeted testing of high-risk segments such as delegated groups, specific specialties, or regions with known accuracy challenges.
Can mock audits focus specifically on delegated provider groups?
Yes. Delegated data is typically where directory accuracy is most variable. Mock audits can be scoped to focus exclusively on delegated groups, with results reported by delegating entity so your team knows exactly where accountability lies.
What happens when the mock audit finds significant issues?
Immediate remediation workflows activate for every flagged provider, with escalation protocols for high-volume or high-severity findings. Executive visibility dashboards show real-time progress so leadership can track resolution before the next CMS audit window opens.
Does this service cover NCQA and state audits as well as CMS?
Yes. The mock audit methodology and documentation package are designed to support CMS secret shopper audits, NCQA credentialing and directory accuracy reviews, and state department of insurance audit requests. One proactive testing cycle produces documentation relevant across all three regulatory audiences.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)

