Custom Provider and Network Surveys for Health Plan Intelligence and Compliance
Custom Design
Built for your specific objective
Independent Execution
Credible, unbiased results
Actionable Reports
Ready for leadership and regulators
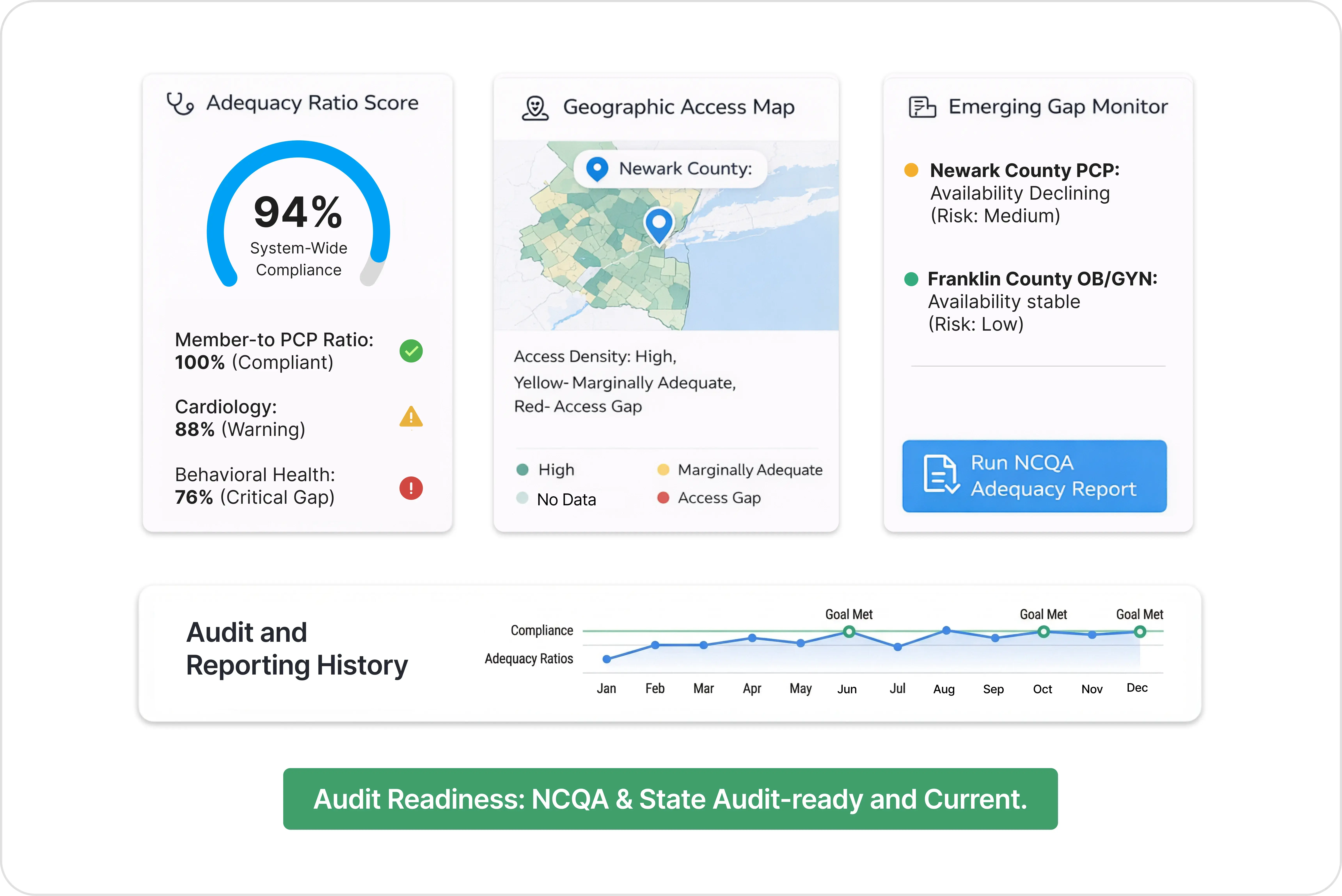
Standard Surveys Answer Standard Questions. Your Network Has Specific Ones.
Gaps Compliance Surveys Don’t Reveal
CMS surveys confirm thresholds, not where access gaps are growing, specialties are strained, or regions are underserved.

Provider Friction Hidden Until It Hurts
Claims and prior auth issues show up late. Provider feedback surfaces operational friction before it impacts revenue.
Attrition Without Clear Signals
Member exits rarely come with reasons. Without structured outreach, you lose insight needed to prevent repeat churn.
PRIME® Designs and Executes Custom Surveys That Produce Network Intelligence
From survey design through statistical analysis and final report, fully managed by Atlas Systems.
[01] Provider Satisfaction Surveys
Understand How In-Network Providers Experience Your Plan
- Surveys in-network providers on claim processing, prior authorization, UM policies, and communication
- Identifies administrative burden points that contribute to provider attrition and network instability
- Measures provider perceptions of plan responsiveness, contracting clarity, and operational support
- Results benchmarked and reported with actionable recommendations for network operations teams

[02] Network Adequacy Assessments
Validate That Your Network Meets Access Standards in Practice
- Assesses provider-to-member ratios, geographic access, and specialty coverage by region
- Measures appointment availability beyond the CMS threshold to surface emerging adequacy gaps
- Identifies specialties and markets where coverage is thinning before they become compliance findings
- Supports NCQA network adequacy documentation and state regulatory reporting requirements

[03] Member Experience Surveys
Capture the Member Experience Before It Becomes Attrition
- Measures member satisfaction with care access, benefit clarity, and plan communications
- Disenrollment surveys capture root cause intelligence from members who have already left
- Covers CAHPS-adjacent dimensions to support quality program planning and Star Ratings improvement
- Results segmented by product line, geography, and member demographic for targeted action

[04] Custom Network Surveys
Design a Survey Around Any Network or Operational Question
- Survey scope, methodology, and outreach protocol designed to your specific objective
- Covers delegation oversight assessments, IPA compliance verification, and provider data accuracy audits
- Layered outreach allows multiple survey purposes to be addressed in a single provider contact
- Delivered with documented methodology, full response data, and statistical analysis

FAQs
How is this different from the CMS Appointment Wait Time Survey?
The CMS Appointment Wait Time Survey is a mandated annual survey with a fixed scope, specific thresholds, and a May 31 submission deadline. Ad hoc surveys are commissioned on demand for any network intelligence objective your plan defines, with no regulatory submission requirement unless you choose to use the results that way.
Can multiple survey objectives be combined into one outreach effort?
Yes. Layering survey purposes reduces provider contact fatigue and is a more efficient use of your provider data. Atlas designs multi-objective outreach programs that gather network adequacy data, provider satisfaction indicators, and compliance verification in a single coordinated effort.
Who typically commissions these surveys?
Network operations leaders use provider satisfaction and adequacy surveys for strategic planning. Quality and compliance teams use them to prepare for NCQA reviews and CMS audits. Medical directors use member experience and disenrollment surveys to inform benefit and care management decisions.
How long does a custom survey take to complete?
Scope determines timeline. A focused provider satisfaction survey for a regional network typically completes in four to six weeks from design to final report. A comprehensive multi-product network adequacy assessment takes eight to ten weeks. Atlas provides a timeline estimate at the scoping stage.




