Payer Enrollment Automation That Moves Providers From Credentialed to Billable Faster
60% Faster
Time to billable status
Zero Manual
Form completion and formatting
One View
All payer relationships tracked centrally
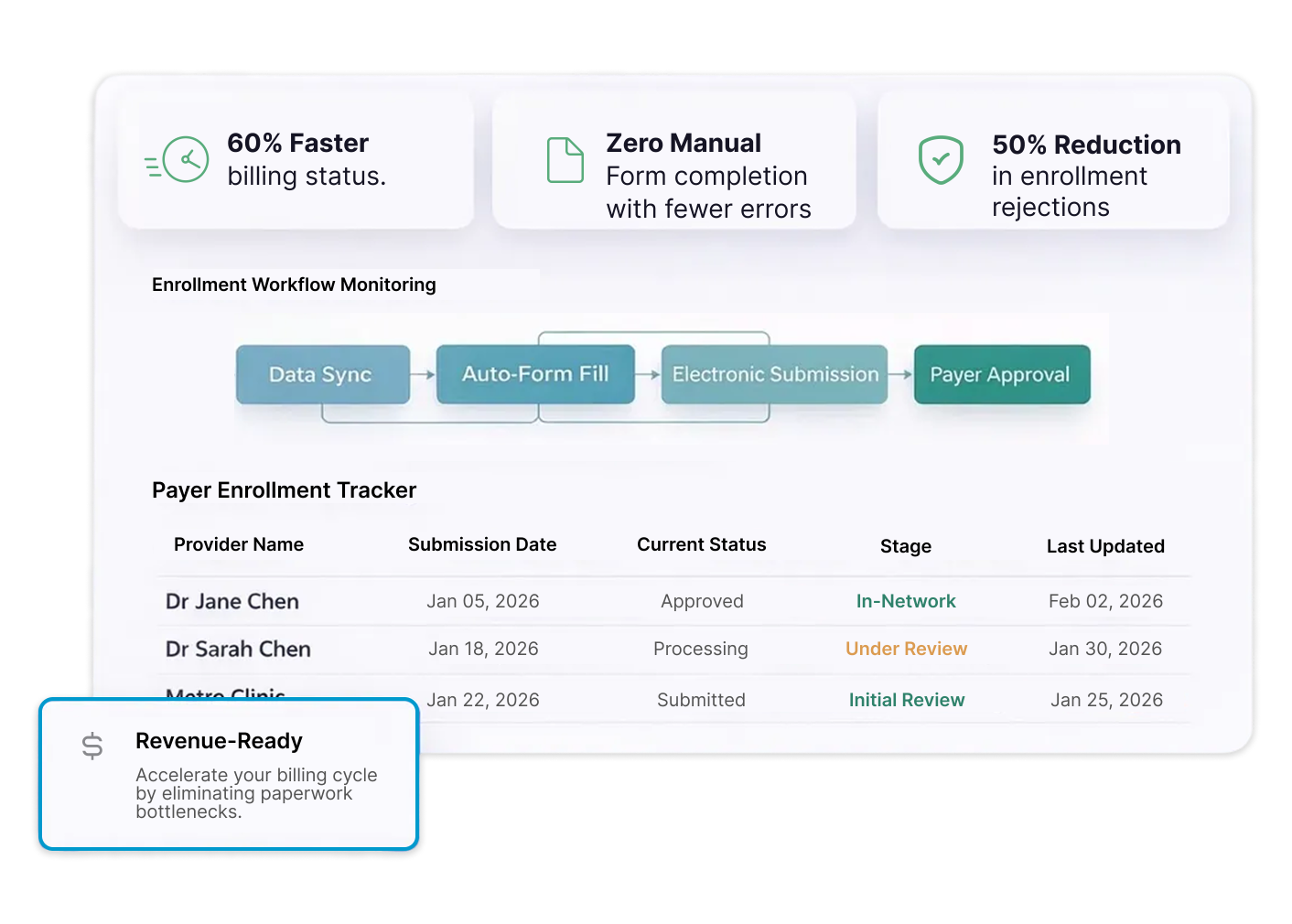
Where Enrollment
Breaks Down
After Credentialing
Same Data. Different Payers. Repeated Work.
The same provider data must be submitted in different formats across every health plan, forcing teams to repeat manual work for each payer relationship.

60–90 Days to Billable Status
Enrollment delays prevent providers from billing for months, holding back revenue and increasing administrative follow-ups.

Rejections Restart the Process
Without structured correction workflows, rejected applications often require full resubmission, extending delays and adding operational strain.
PRIME® Streamlines Payer Enrollment Alongside Credentialing Workflows End-to-End.
One governed workflow connects provider records directly to payer submissions, so enrollment runs in parallel with credentialing rather than after it.
[01] Automated Application Generation
Payer-Specific Submissions Without Manual Formatting
- Pulls verified provider data directly from the PRIME® Provider Data Engine for each application
- Formats applications automatically to each payer's required structure, EDI, portal, or flat file
- Covers major commercial payers, Medicare PECOS, state Medicaid portals, and managed care programs
- Pre-submission validation catches missing fields and format errors before transmission

[02] Simultaneous Multi-Payer Submission
Submit to All Payers at Once, Not One at a Time
- Triggers enrollment submissions to all relevant payers as soon as credentialing is complete
- Tracks each submission independently with payer receipt confirmation and processing stage
- Alerts on delayed applications approaching 90 days without a decision for proactive follow-up
- Submission date, expected decision timeframe, and current status visible in one centralized view

[03] Rejection Resolution
Correct and Resubmit Without Rebuilding
- Captures specific payer rejection reasons with full submission context automatically
- One-click resubmission sends corrected applications without rebuilding the entire record
- Surfaces rejection patterns across multiple providers with the same payer for systemic fixes
- Tracks rejection rates and resolution times per payer to identify recurring bottlenecks

[04] Enrollment Status Visibility
Every Payer Relationship, One Dashboard
- Centralizes enrollment status across all providers and all payers in a single view
- Filter by provider, payer, enrollment stage, submission date, or product line
- Payer performance dashboard tracks response times, load turnaround, and approval cycle KPIs
- Exportable reports give leadership visibility into overall enrollment pipeline health at any point
Payer Enrollment Automation Software - FAQs
What is payer enrollment software?
Payer enrollment software automates the process of registering healthcare providers with insurance networks so they can bill and receive reimbursement. It centralizes provider data, auto-fills payer-specific applications, integrates with CAQH, tracks submission status across every payer, and manages document expirations and recredentialing reminders. Strong platforms reduce enrollment timelines from 90 to 150 days down to 30 to 60 days while eliminating manual paperwork.
How does PRIME® trigger enrollment after credentialing is complete?
PRIME® connects the credentialing and enrollment workflows directly. When a provider completes initial credentialing, enrollment submissions trigger automatically for all relevant payers without a manual handoff between teams. Provider data flows from the credentialing record into applications with no duplicate entry.
Which payers and programs does PRIME® support for enrollment?
PRIME® supports enrollment with major commercial health plans, Medicare PECOS, state Medicaid portals, and managed care programs. Payer-specific templates are maintained and updated as requirements change, so submissions always meet current specifications without manual format monitoring.
What is the difference between non-delegated and delegated enrollment?
Non-delegated payer enrollment is where a provider organization submits applications directly to health plans to establish billing eligibility and network participation. Delegated enrollment is where a health plan manages credentialing and enrollment on behalf of provider groups.
What happens when a payer rejects an application?
PRIME® captures the specific rejection reason, logs it with the full submission context, and queues the enrollment for correction. Once the provider record is updated, corrected applications can be resubmitted without rebuilding from scratch. Rejection patterns that affect multiple providers with the same payer surface automatically for systemic resolution.
Can we track enrollment across multiple product lines simultaneously?
Yes. The enrollment dashboard filters by provider, payer, product line, submission date, and enrollment stage. Plans managing Medicare Advantage, Medicaid, and commercial enrollment simultaneously have full visibility across all three from a single view.
How does payer enrollment software work?
The software pulls verified provider data from a centralized profile or CAQH integration, then auto-fills enrollment applications for each payer using payer-specific templates. It transmits submissions through the payer's preferred channel including PECOS for Medicare, state Medicaid portals, or direct payer integrations. Real-time dashboards track application age and approval status, automated reminders flag revalidations and document expirations, and audit trails log every submission, payer response, and approval decision.
What features should you look for in payer enrollment software?
Evaluate whether the platform offers CAQH integration, payer-specific application templates, centralized provider profiles, automated submission tracking across every payer, and configurable reminders for revalidation and document expirations. Check coverage depth: leading platforms support 4,000+ payers including Medicare PECOS, state Medicaid portals, commercial insurers, Tricare, and VA Community Care. Confirm audit trail completeness, integration with credentialing and billing systems, and whether the platform handles group, individual, and multi-tax-ID enrollment on the same workflow.
Can software handle Medicare and Medicaid enrollment, or just commercial payers?
Strong platforms handle all three, but the workflows are different. Medicare enrollment runs through the PECOS portal with specific revalidation cycles, Medicaid varies by state with 50 different submission requirements, and commercial payers each have their own application formats. Look for software that maintains current PECOS workflows, supports all 50 state Medicaid portals, and includes Tricare and VA Community Care if your network needs them. Software that only handles commercial payers will leave significant gaps.
Does payer enrollment software integrate with CAQH?
Yes, this is one of the highest-value integrations because most commercial payers pull provider data directly from CAQH ProView. Strong platforms sync provider profiles bidirectionally with CAQH, so updates made in one system flow to the other automatically. This eliminates duplicate data entry, reduces application errors caused by stale CAQH profiles, and keeps the most-used commercial payer source of truth current without manual intervention.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)

