Meet CMS Appointment Wait Time Requirements With an Independent Secret Shopper Survey Service
Meet 90% Compliance
Required CMS threshold
Independent Third Party
As mandated by CMS
Audit-Ready Reports
Submitted by May 31 Deadline
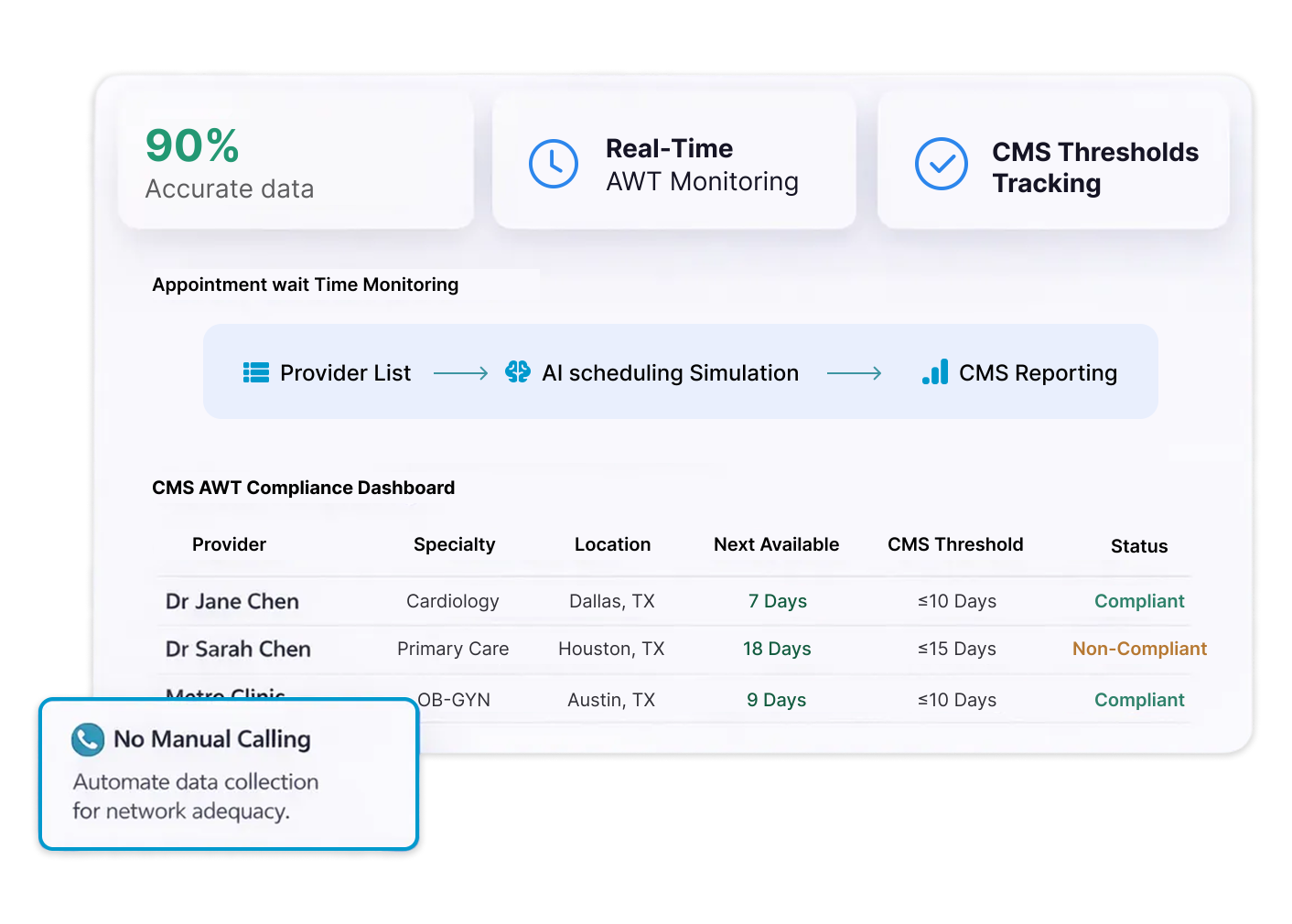
CMS Compliance Now Requires Third-Party Survey Execution
A Mandate With No In-House Option
CMS requires health plans to use an independent third party for appointment wait time surveys. Plans that conduct surveys internally are non-compliant regardless of the results they report.

Three Provider Types, Three Different Standards
Primary care, behavioral health, and specialist appointments each carry different wait time thresholds. Meeting 90% compliance across all three simultaneously requires a structured, coordinated survey program, not ad hoc outreach.
A Hard Deadline Every Year
Survey results must be submitted to CMS by May 31 annually. Plans that start late or manage the process manually risk missing the window entirely, triggering penalties and audit exposure.
PRIME® Runs Your Secret Shopper Survey, Fully Managed
Over 20 years of experience conducting appointment wait time surveys for health plans across all product lines.
[01] Survey Design
Tailored Scripts and Outreach Protocols
- Survey scripts designed for primary care, behavioral health, and specialist appointments separately
- Covers both in-person and telehealth appointment availability as required by CMS
- Outreach protocols adapted to different product lines including Medicare, Medicaid, and commercial
- Scripts validated against CMS requirements before survey launch

[02] Independent Outreach
Third-Party Execution CMS Requires
- Atlas conducts all outreach independently with no affiliation to the health plan being surveyed
- Verifies whether providers are in-network, accepting new patients, and meeting wait time standards
- Covers the full survey window from January through May annually
- Documents every outreach attempt with call logs, outcomes, and timestamps

[03] Wait Time Measurement
Primary Care, Behavioral Health, and Specialists
- Measures compliance against 15-business-day standard for primary care appointments
- Measures compliance against 10-business-day standard for behavioral health appointments
- Measures compliance against 30-business-day standard for specialist appointments
- Tracks results in real time across all provider types and geographies simultaneously

[04] Analysis and Reporting
Audit-Ready Results by May 31
- Statistical analysis meets CMS methodology requirements for representative sampling
- Results compiled into CMS-ready report format with documented compliance rates by category
- Full documentation of survey methodology, outreach evidence, and exception handling
- Delivered with sufficient lead time for internal review before CMS submission deadline

FAQs
Why can't we conduct this survey in-house?
CMS requires that appointment wait time surveys be conducted by an independent third party with no affiliation to the health plan. Surveys conducted internally do not satisfy the mandate regardless of methodology or results.
Which product lines does the survey need to cover?
Survey requirements vary by product line. Medicare Advantage, Medicaid managed care, and QHP plans on federal exchanges each have specific survey protocols and reporting requirements. Atlas designs separate outreach programs for each line of business your plan operates.
What happens if a provider does not respond to outreach attempts?
Non-response is documented with call log evidence and handled according to CMS guidance on minimum contact attempts. Atlas tracks and reports non-response rates as part of the full survey documentation package.
When does the survey need to start to meet the May 31 deadline?
Survey outreach typically runs from January through April, with statistical analysis and report compilation completed in May. Plans that engage Atlas before the January window receive priority scheduling and adequate time for internal review before submission.
Can Atlas help if we receive audit findings after submission?
Yes. Atlas supports corrective action planning, documentation review, and re-survey services for plans that receive findings following CMS review.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)

