Provider Credentialing Software for Credentialing, Recredentialing, and Ongoing Compliance
70% Faster
Credentialing cycles
Zero Missed
Credential expirations
Continuous
Compliance monitoring
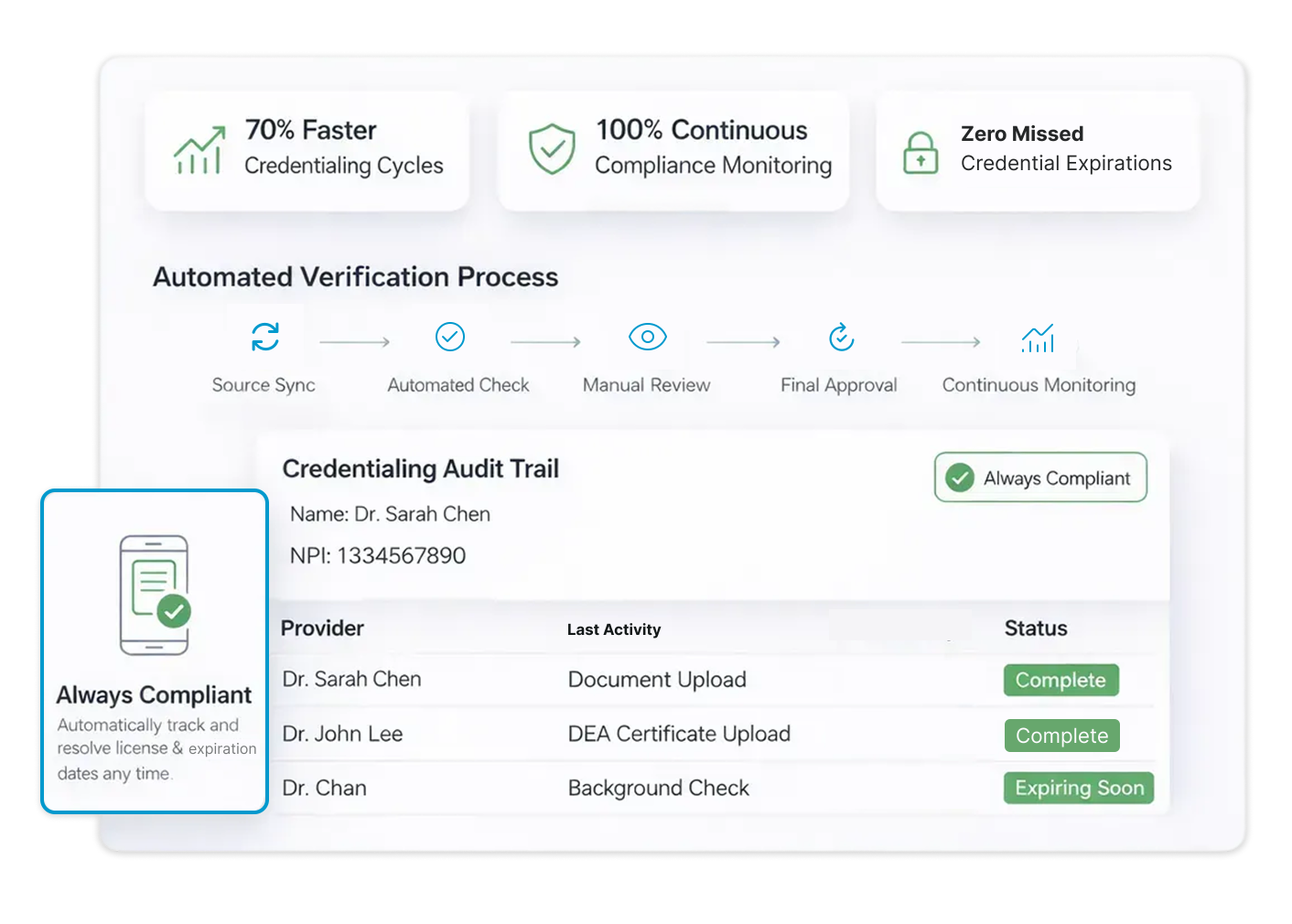
Credentialing isn’t one step. It’s ongoing.
Most platforms treat it like a one-time task.
Manual Verification Across Dozens of Sources
Credentialing requires checks across state boards, DEA, OIG, and specialty bodies. Each tracked separately. Each prone to delays that impact care and revenue.
Re-Credentialing That Catches Teams Off Guard
Three-year cycles only work if workflows start 90 days early. Without automation, deadlines slip and compliance gaps emerge.
Compliance Events Between Cycles
Licenses change. Sanctions happen. Without continuous monitoring, issues surface only during audits or claim denials.
One platform covers every stage, from initial verification through re-credentialing to continuous monitoring, so nothing falls between cycles.
[01] Primary Source Verification
Automated Credential Verification at Onboarding
- Verifies licenses against state medical boards, nursing boards, and allied health registries
- Confirms board certifications through ABMS, AOA, and specialty board databases
- Screens simultaneously against OIG, SAM.gov, NPDB, DEA, and all 50 state exclusion lists
- Routes malpractice history, hospital privilege, and work history inquiries automatically

[02] Re-Credentialing
Scheduled Re-Verification at Every Cycle
- Initiates re-credentialing workflows automatically 90 days before each cycle due date
- Runs the same primary source verifications as initial credentialing with updated source data
- Tiered expiration alerts notify providers, credentialing teams, and leadership at 90, 60, and 30 days
- Bulk expiration reports enable proactive workload planning across your entire provider network

[03] Expiration Management
Track Every Credential Across Every Provider
- Monitors license renewal dates, DEA registration expiry, and board certification windows
- Configurable alert rules adapt to your organization's lead time requirements by credential type
- Automated reminders to providers, credentialing teams, and leadership prevent lapses before they occur
- Zero missed expirations across networks of any size without manual tracking spreadsheets

[04] Continuous Monitoring
Compliance Oversight Between Credentialing Cycles
- Monitors licensure status, sanctions, and credentialing data continuously between cycles
- Flags new disciplinary actions, DEA expirations, and board certification lapses immediately
- Detects compliance events that a three-year re-credentialing cycle would not catch until too late
- Automated alerts route to the right team the moment a change is identified at any source

Complete Documentation
- Primary source verification records with source attribution, verification date, and next due date per credential
- Re-credentialing packages with complete evidence for NCQA, Joint Commission, and CMS requirements
- Expiration tracking logs documenting alert issuance, provider response, and renewal confirmation
- Continuous monitoring records capturing every compliance event detected, alert routed, and resolution confirmed

Provider Credentialing Software - FAQs
How does automated credentialing differ from manual primary source verification?
PRIME® queries official databases directly and receives responses in hours or days. Manual verification through phone calls, faxes, and mailed requests typically takes two to four weeks per source, with higher error rates from manual data entry on the return.
When does the re-credentialing workflow initiate?
PRIME® automatically initiates the re-credentialing workflow 90 days before each provider's cycle due date. Document collection, primary source re-verification, and reviewer routing all happen within the platform, with tiered alerts escalating at 60 and 30 day if any step remains incomplete.
Does PRIME® handle providers credentialed in multiple states?
Yes. PRIME® verifies and monitors licenses independently across every state where a provider holds an active license, with each jurisdiction's requirements tracked separately and alerts issued per credential rather than per provider.
What compliance standards does the documentation support?
PRIME® generates audit-ready documentation for CMS Medicare and Medicaid requirements, NCQA credentialing and re-credentialing standards, Joint Commission primary source verification requirements, and state-specific jurisdiction timelines.
How does continuous monitoring relate to re-credentialing?
Re-credentialing is a comprehensive point-in-time verification that runs on a defined cycle. Continuous monitoring is what protects your organization between those cycles, catching sanctions, license lapses, and disciplinary actions before they affect patient care, payer standing, or claims processing.
What is provider credentialing software?
Provider credentialing software automates the verification, enrollment, and ongoing monitoring of healthcare providers' qualifications. It handles primary source verification against state medical boards, NPPES, OIG exclusion lists, and DEA registries, manages NCQA-aligned workflows, tracks license expirations, and maintains complete audit trails, reducing credentialing turnaround times by up to 70% compared to manual spreadsheet-based processes.
How does provider credentialing software work?
The software collects provider applications through digital forms or CAQH integration, then runs automated primary source verification against authoritative databases including state medical boards, NPPES, OIG LEIE, SAM.gov, and DEA. It routes exceptions to human reviewers, tracks committee approvals, and pushes verified records to credentialing, directory, and claims systems. Continuous monitoring runs in the background between recredentialing cycles, flagging sanctions, license lapses, and disciplinary actions the moment they appear.
What features should you look for in provider credentialing software?
Evaluate whether the platform offers automated primary source verification, NCQA-aligned workflows, continuous sanctions and license monitoring, CAQH integration, configurable committee approval routing, and complete audit trail documentation. Integration depth matters, so check for bidirectional sync with your directory, claims, and enrollment systems. Also confirm the platform supports both initial credentialing and recredentialing on the same workflow, and that implementation can be completed in weeks rather than quarters.
How long does credentialing take with credentialing software?
Manual credentialing typically takes 90 to 150 days per provider. Purpose-built credentialing software reduces this to 30 to 60 days by automating primary source verification, eliminating manual form routing, and flagging exceptions in real time. PRIME® customers see up to 70% faster credentialing cycles by collapsing parallel verification steps that would otherwise run sequentially.
Is provider credentialing software the same as payer enrollment software?
No. Credentialing verifies a provider's qualifications through primary source checks, which payers use for network inclusion and compliance. Payer enrollment is the separate process of registering a credentialed provider with specific health plans so they can bill for services. Strong platforms like PRIME® cover both on a unified workflow, so verified credentials flow directly into enrollment submissions without duplicate data entry.
How is PRIME® different from other provider credentialing software?
PRIME® runs credentialing, recredentialing, and continuous compliance monitoring on a single platform rather than across separate products. It screens providers daily against OIG LEIE, SAM.gov, and all 50 state Medicaid exclusion lists, so sanctions surface between cycles rather than during the next review. Credentialing workflows deploy in under four weeks, NCQA alignment is built in, and every verification step creates timestamped audit documentation that stays audit-ready at any moment.


-1.png?width=387&height=387&name=IDC%20Banner%20(1)-1.png)


.png?width=1030&height=152&name=Group%202087329257%20(2).png)